目次を確認
【マネフレ現金化】クレジットカード現金化♪カードでお金ならマネフレ!

※マネフレのサイト紹介の動画をご覧ください!
▼クリックすると動画が読み込まれます。▼
【YouTube動画チャンネル】
クレジットカード現金化ならマネフレはコチラへ

-
 ソニックマネー
ソニックマネー 詳細を見る換金率99.2%最短3分
詳細を見る換金率99.2%最短3分他社様からお乗り換えがお得!
-
 OKクレジット
OKクレジット 詳細を見る換金率99.7%最短3分
詳細を見る換金率99.7%最短3分スマホで超簡単で日本一安全な現金化!
-
 トラストキャッシュ
トラストキャッシュ 詳細を見る換金率99.5%最短15分
詳細を見る換金率99.5%最短15分幅広いクレカ金融機関で対応可能!
クレジットカードから現金化でお金ができる方法を教えてほしい
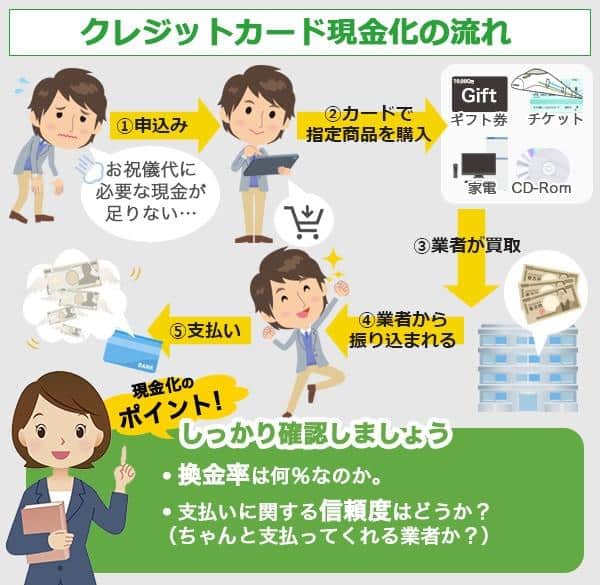
クレジットカード現金化とは

クレジットカード現金化業者に依頼をしてショッピング枠を買い取ってもらうことになります。
ただ、直接買い取ってもらうと本来の利用目的から外れてしまう問題があるため、クレジットカードで業者が指定する商品を購入した後、業者から現金を振り込んでもらえるようになっているのが一般的です。
【お金の友達】マネーフレンドの細かい調査で金策のサービスを提供する

マネーフレンド≪お金の友達≫とは急な出費でお金に困っている人たちをサポートするクレジットカード現金化を比較するランキングサイトです。
一般のユーザーが疑う不法な取引や違法性などは一切ございません!
現金化のポータルサイトとして7年目の実績とお客様の信頼と利用するリピーターからも信用されている『マネフレ』を今後ともよろしくお願い致します!
マネーフレンドのマネーサービス詳細情報
マネーフレンドとは
当サイト『マネフレ』は、闇金融・貸金業を行う業者ではなく、現金化をサポートしている比較ランキングサイトです。
マネフレとはマネーフレンド≪お金の友達≫の通称『マネフレ』の愛称として多くの現金化利用の人に愛されサイト運営実績も9年目に突入しております!
これもお金に困っている人たちをサポートし続けて勝ち取った信頼の証とも言えるのではないでしょうか。
これからも急な現金が必要な人の助け舟となるよう日々邁進し、お客様第一をモットーとして考えながら日々お金に役立つポータルサイトとして運営していきたいと思います!

古物商として買取を行う現金化について

マネフレのクレジットカード現金化とは、厳密にはクレジットカードの「ショッピング枠」の現金化のことです。
利用者は現金化業者からクレジットカードで品物を購入し、その品物を現金化業者に買い取ってもらうことで現金を手にすることができるというシステムです。
業者はお金を貸したり(融資)ではなく、古物営業法に基づき「古物商」として買取を行っているというスタンスで営業しています。
実際に品物分の料金請求はクレジットカード会社から発生し、翌月分の料金として引き落としされます。
利用者がカードをリボ払いや分割払いに設定していれば、それに応じて買い物をした分の代金の支払いがなされることに。
現金化には大きく分けてキャッシュバック方式と買取方式があります。
キャッシュバック方式は、利用者が業者指定の商品を購入すると、手数料を引いた金額がキャッシュバックとして振り込まれます。
買取方式は、利用者が指定の商品を購入すると、現金化業者が手数料を差し引いた金額で買い取るというものです。
>>現金化の仕組み 還元率・換金率などの詳細はコチラ
現金化の申込方法と振込までの流れをチェックしてみよう!

マネフレによる現金化の方式は先述のとおり。
では実際にクレジットカードの現金化を審査なしで申し込むとどういった手順で現金を手にすることになるのでしょうか。
現金化の申込の多くは電話かサイトの申込フォーム、メールなどで行います。多くの会社ではWeb申込からだと24時間対応しています。

その後本人確認などの確認作業が完了したら、現金化業者の指定するサイトにアクセスし、商品をカード決済で購入します。
各現金化業者では還元率を設定しており、還元率に基づいた金額から手数料を差し引いた額が利用者の口座に振り込まれます。

利用者の口座によっては業務時間外だと翌日付での送金になる場合もありますが、現金化業者と提携している銀行のネットバンキングなどに口座があれば24時間入金確認ができます。
クレジットカード現金化は違法なのか?リスクを調査

マネフレの現金化サービスは貸金業・融資ではなく古物商というくくりで営業を行っています。
商品の受け渡しが目的という名目で現金を振込むのはオプションという形。

もっとも、クレジットカード会社の規約では換金を目的としてショッピング枠を利用することは違反にあたります。
ただしこれも換金目的かどうかという利用者の意志を特定することは難しいため、実際にカード会社から規約違反で強制解約を強いられるケースはごくごくまれであると言えるでしょう。
それ以上に気を付けなければいけないのは、便利だからといって必要以上に来店不要で審査がいらない現金化を利用してしまうこと。
また詐欺まがいの換金率を提示する悪徳業者も紛れ込んでいますから、十分な注意が必要です。
クレジットカード現金化の診断チェック!
- Q1
- 個人?法人?